
Image by Denzel Boyd, graphic by Rebecca Russ, for COURIER.
Medicine and science have historically abused or dismissed Black people. Now, Black doctors are working hard to reverse the COVID-19 vaccine hesitancy Black Americans rightfully have as a result.
Candace Dru strives to live a holistic lifestyle and promotes healthy living to the clients she serves as a certified lactation counselor and student midwife. She makes conscious choices for herself and her son to consume what she says is high-quality food as a natural immune system boost.
“I’m a person who researches everything, and I’m all about informed consent and informed refusal,” Dru said. “People need time to research the vaccine, and they should be educated on its actual benefits.”
Those are among the reasons why she’s chosen not to take the COVID-19 vaccine. Distrust is another. Dru, of Columbia, S. C., thinks the vaccine was created too fast. As a person who reads the ingredient list for anything she consumes, she also doesn’t trust a vaccine whose composition she hasn’t been able to access.
Sorting Fact From Fiction: Sign Up for COURIER’s newsletter.
Dru is far from alone in her hesitancy. Black Americans are 3.7 times more likely to be hospitalized and 2.8 times more likely to die from the coronavirus but have consistently exhibited the most reluctance toward getting the vaccine. In a December Axios-Ipsos poll, just 16% of Black Americans surveyed said they would get the vaccine as soon as it was available. Two months earlier, only 5% said they would. In comparison, 29% of white and 22% of Hispanic respondents said they would receive the vaccine.
The same month, a Kaiser Family Foundation study found that 35% of Black adults said they “definitely or probably” would not get vaccinated, compared to 26% for white and Hispanic adults. Among the Black adults who said they definitely or probably wouldn’t take the vaccine, 47% said they didn’t trust vaccines in general, and 50% were worried they could contract the coronavirus from the vaccine.
Years of research and a brand-new technology called mRNA have allowed scientists to create COVID-19 vaccines quicker than vaccines of the past. Still, many Americans are hesitant—and Black doctors are doing their part to validate Black Americans’ distrust while working to gain that trust back.
A History of Medical Racism and Abuse
Vestiges of the Tuskegee Study still linger as evidence of mistreatment by the medical establishment. Black men who participated in the study from 1932 until the Department of Health and Human Services ended it in 1972 believed they were receiving treatment for their syphilis when they were being studied and left untreated. Even when penicillin was widely available and effective, the men were left to die while scientists studied their symptoms and lives. In another case of non-consent, the cells of Henrietta Lacks, a Black Baltimore woman with cervical cancer in 1951, were taken by Johns Hopkins Hospital to be used for research when she went for treatment. These cells, called HeLa cells, were used in COVID-19 research to help scientists develop a vaccine. Lacks died destitute even though her cells are considered by many to be the “foundation of modern medicine.”
Medical abuse has a long history. Dr. J. Marion Sims, considered the father of modern gynecology, experimented on enslaved Black women without their consent or anesthesia. He then took the techniques and surgeries he perfected on Black women’s bodies to perform them with pain management on white women. The list of racial injustices in medicine and science goes on. Black Americans seeking medical treatment also don’t have to look to the past to find instances of systemic bias and racism.
The COVID-19 related death of Dr. Susan Moore, a Black doctor who posted a video to social media from her hospital bed detailing how white doctors and nurses treated her, serves as a prominent recent example. That’s why a growing number of Black medical professionals are choosing to take the vaccination message directly to Black communities.
Developing Trust
The National Medical Association, the largest and oldest national organization representing Black physicians and their patients in the United States, launched a task force to examine the safety and effectiveness of COVID-19 treatments, including the vaccine. The NMA ultimately supported FDA approval of emergency use authorization for the Pfizer and Moderna vaccines while advocating for “culturally sensitive, multilingual outreach” to address health outcome gaps.
The Black Coalition Against COVID-19—a collaborative of health care professionals, medical organizations, medical school, and community leaders—composed a Love Letter to Black America to address concerns and alleviate fears about coronavirus treatment.
“We approach this work by acknowledging historical issues around medical research with African Americans in the US and focus on the current state of research and health care in our communities,” said Martha Dawson, assistant professor at the University of Alabama at Birmingham School of Nursing and president of the National Black Nurses Association, Inc.
Dawson, one of the organizers of the Black Coalition Against COVID-19, said Black healthcare providers have a responsibility to care for the outcomes of Black Americans “with their heads and their hearts” in light of the historical issues involved. “We know that improvement is still needed to improve health equity and quality of care in Black communities,” she said. “We are transparent about what scientists are telling us about COVID-19, what we don’t know, and what we are learning.”
Other healthcare providers are using social media to alleviate fears and concerns. Dr. Oluseyi A. Fadayomi, a Maryland-based pain specialist, posted a video to his Instagram account for his followers showing him receiving the vaccine.
Fadayomi said he posted his own process of getting the vaccination on social media because it’s important for others to know the vaccine is safe. “Before I got the vaccine, I did my own due diligence. I looked at the data, the methodology, the reports coming from authorities and from the country’s medical leaders stating the vaccine was safe,” he said. “I trusted the vaccine and knew it was going to be okay.”
As a Black doctor, Fadayomi said it was important to add his voice to the vaccine conversation after talking to hesitant friends. He said the video helped alleviate some of their concerns and reluctance to get the vaccination. One person said they weren’t going to get the vaccine initially but now planned to do so. He said another friend who had seen a video of a nurse fainting after receiving the vaccine believed she had died and worried that he too would suffer a tragic fate. Seeing Fadayomi’s Instagram post calmed her fears and started a conversation that helped dispel misinformation online.
“The greater good is the protection of everybody in the country,” he said. “This virus is a serious illness and has killed a lot of people, especially people of color.”
As of Jan. 8, at least 55,088 Black Americans had died of COVID-19, according to The COVID Racial Data Tracker, accounting for 16% of all COVID-19 deaths. Close to 370,000 Americans overall have died from the virus.
A Multifaceted Approach
Dru said she would be open to inoculation against COVID-19 so she can be safe while caring for pregnant and breastfeeding people. Still, she would like to learn more about the vaccine’s effectiveness against newer strains of COVID-19 and how the vaccine would affect pregnant and breastfeeding people—especially since the vaccine wasn’t tested on that population.
“What we need more than anything is access to healthcare to address the health disparities in the Black community,” she said.
As Black medical providers work to promote COVID-19 vaccination in Black communities, they recognize that addressing the history of medical racism and working to increase the percentage of Black healthcare providers will ultimately make the difference in decreasing COVID-19 hospitalizations and deaths—vaccine or not.
“Scientists and medical professionals must own their history and step forward to engage with the Black community when there is not a Hurricane Katrina or a pandemic,” said Dawson, the National Black Nurses Association president. “They should work with us to address health inequities and disparities by joining with social, community, and health care groups to improve access to health services and work to address the social determinants of health.”
READ MORE: Three Americans Share Why They Volunteered For COVID Vaccine Trials
Politics

Infrastructure funding to help repair two historic Philadelphia bridges
Philadelphia is set to receive $14.2 million from President Joe Biden’s infrastructure law to repair two historic bridges crossing the Wissahickon...

Biden cancels student loan debt for 10,800 more Pennsylvanians
The Biden administration on Friday announced its cancellation of an additional $7.4 billion in student debt for 277,000 borrowers, including 10,800...

The Republican war on Medicare raises the stakes in 2024
Nearly 3 million Pennsylvanians rely on Medicare benefits—benefits they spent decades paying into, with the promise that the program would be there...
Local News
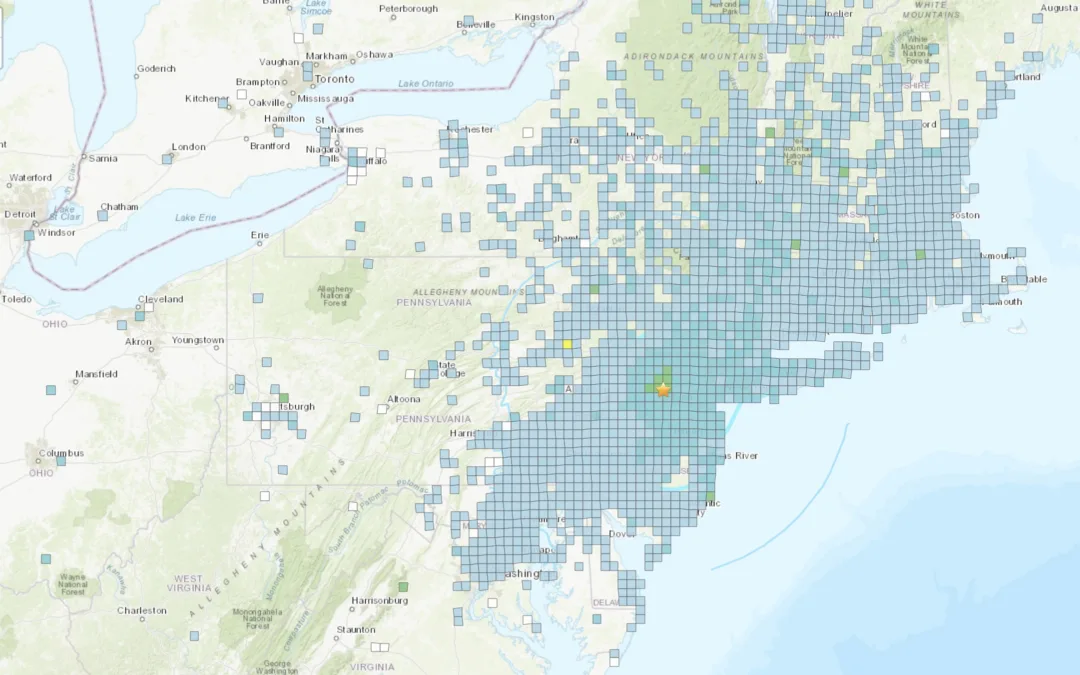
4.8 magnitude earthquake centered in New Jersey felt across Pennsylvania Friday morning
According to the U.S. Geological Survey, the quake’s impact in Pennsylvania was primarily felt in the eastern part of the state, though the...

‘SCTV’ star Joe Flaherty, a Pittsburgh native, has died at 82
Flaherty established himself while working with Eugene Levy, Martin Short, and Catherine O’Hara on the classic Canadian sketch comedy show, and...





