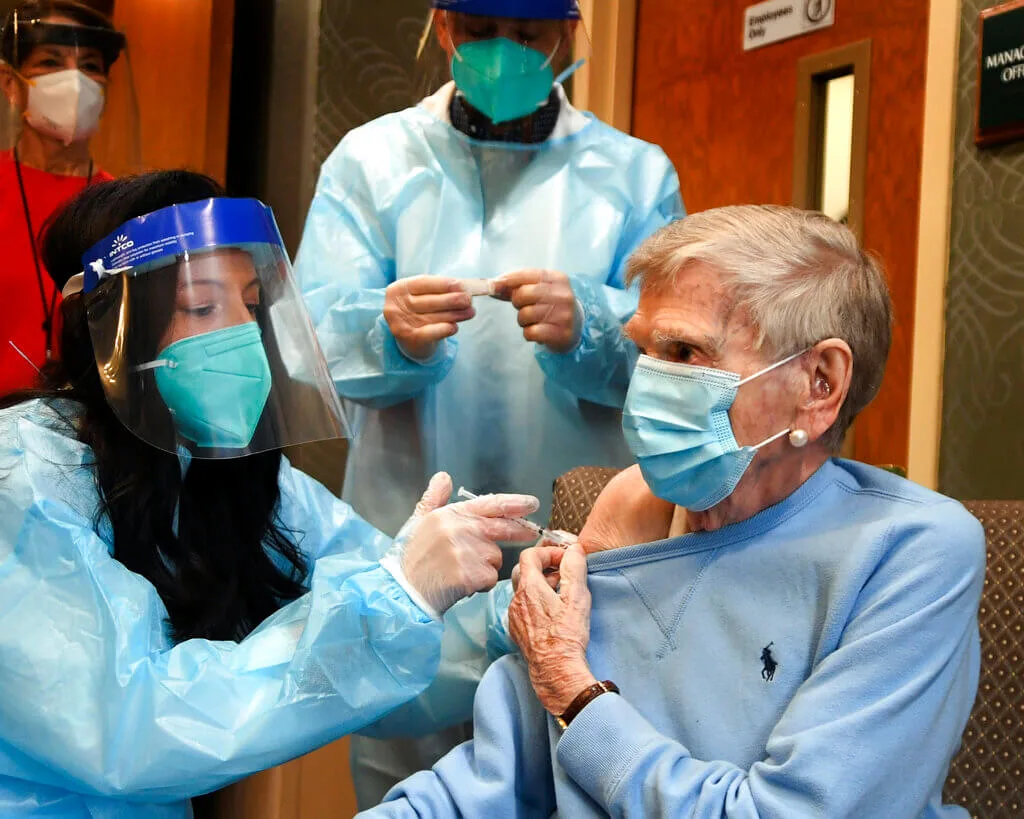
Mary Lou Galushko gives Jeanne Peters, 95, a rehab patient at The Reservoir, a nursing facility, the first COVID-19 vaccination at the nursing home Friday, Dec. 18, 2020, in West Hartford, Conn. (AP Photo/Stephen Dunn, Pool)
The group recommends protecting those among the most likely to contract the virus: workers who can’t work from home and older Americans who have represented a disproportionate percentage of hospitalizations and deaths.
As the United States continues its campaign to vaccinate frontline healthcare workers, a Centers for Disease Control and Prevention (CDC) panel on Sunday voted to recommend that people ages 75 and older and frontline essential workers be next in line for vaccinations.
The CDC’s Advisory Committee on Immunization Practices agreed to prioritize the roughly 30 million frontline workers and 21 million people over the age of 75, including 2 million who overlap as frontline workers, for the next phase (Phase 1b) of vaccination, which is expected to begin in January.
The vote came amid increasingly contentious debate over which populations should get vaccinated first as the US outbreak reaches its most dangerous point yet. The US is recording over 2,600 deaths and more than 210,000 cases per day over the past week, according to the COVID Tracking Project. In total, nearly 320,000 people have died of COVID-19 in the US, while more than 17 million have been infected.
Sort Fact From Fiction: Sign up for COURIER’s Newsletter
By selecting these groups, the CDC appears to prioritize protecting those most likely to contract and transmit the virus: workers who can’t work from home and older Americans who have represented a disproportionate percentage of hospitalizations and deaths. According to the latest CDC data, adults 75 years and older make up less than 7% of the US population but account for 25% of COVID-19-associated hospitalizations and 59% of deaths.
“I feel very strongly we do need to have that balance of saving lives and keeping our infrastructure in place,” Dr. Helen Talbot, a member of the panel and an infectious-disease specialist at Vanderbilt University, said during the virtual meeting. “It’s easy for us to give vaccines in our clinics. It’s not easy for us to give vaccines to the people on the front lines, for multiple reasons.”
The recommendations came just two days after the US Food and Drug Administration provided emergency authorization for a coronavirus vaccine from Moderna, which is the second to be approved following Pfizer-BioNTech’s vaccine. Roughly 6 million doses of the Moderna vaccine are expected to be distributed across the country this week, according to the Washington Post. More than 2.8 million doses of the Pfizer vaccine have already been distributed, and 556,208 of those shots have been administered as of Sunday afternoon, according to the CDC.
RELATED: All Vaccines Have Side Effects. The COVID Vaccine Is No Different. What You Need to Know.
As caseloads spiral across much of the country, the federal government has said it anticipates having enough doses to inoculate around 100 million people in the US by the end of February. The agency also hopes to reach Phase 1c sometime in February. During Phase 1c, access to vaccines would expand to include 129 million more people, including adults ages 65 to 74, adults with preexisting medical conditions, and other essential but non-frontline workers, such as those who work in food service and construction. All other Americans are expected to have to wait until the spring or early summer to receive a vaccine.
The phases are more of a guideline than a strict rule, however, and they could even overlap. “It is not necessary to fully complete vaccination in one phase before moving to the next phase,” the CDC’s Sara Oliver told NPR.
State and local governments also retain flexibility to adjust their priorities and determine which groups receive vaccines first.
RELATED: Pence’s Vaccine PR Stunt Isn’t Helping States Scrambling to Get Doses
Members of the CDC panel did warn that the federal government needs to provide additional funding to state and local health departments to ensure that distribution is carried out smoothly and quickly.
“The fact that the state and local health departments have not been funded for vaccination program, especially in the context of the billions of dollars that funded the extremely successful program to develop vaccines is really appalling,” said Dr. Beth Bell, who voted “yes” on the proposal.
“Today, state and local health departments are on life support,” added Dr. Jeffrey Duchin, a panel member who is in charge of public health in Seattle and King County, Washington. “We’re hamstrung and stymied by the lack of necessary federal funding to allow us to take advantage of these newly available vaccines.”
Congress appears to be on the verge of providing such funding. Leaders of both parties agreed to a new round of coronavirus relief on Sunday. Should that bill pass the House, Senate, and be signed into law by President Donald Trump, it would include $20 billion to purchase vaccines and $8 billion for distribution.
CDC Director Dr. Robert Redfield will review the panel’s recommendation and decide whether to support it as the agency’s official state guidance.
UPDATE (December 22, 2020, 10:13 a.m.): This story has been updated to reflect that adults 75 and older account for 59% of COVID-19 deaths.

For Rep. Susan Wild, supporting PA families includes reproductive rights and much more
Rep. Susan Wild wants to be very clear with Pennsylvanians: Donald Trump is committed to taking away women’s reproductive freedom, but he is not...
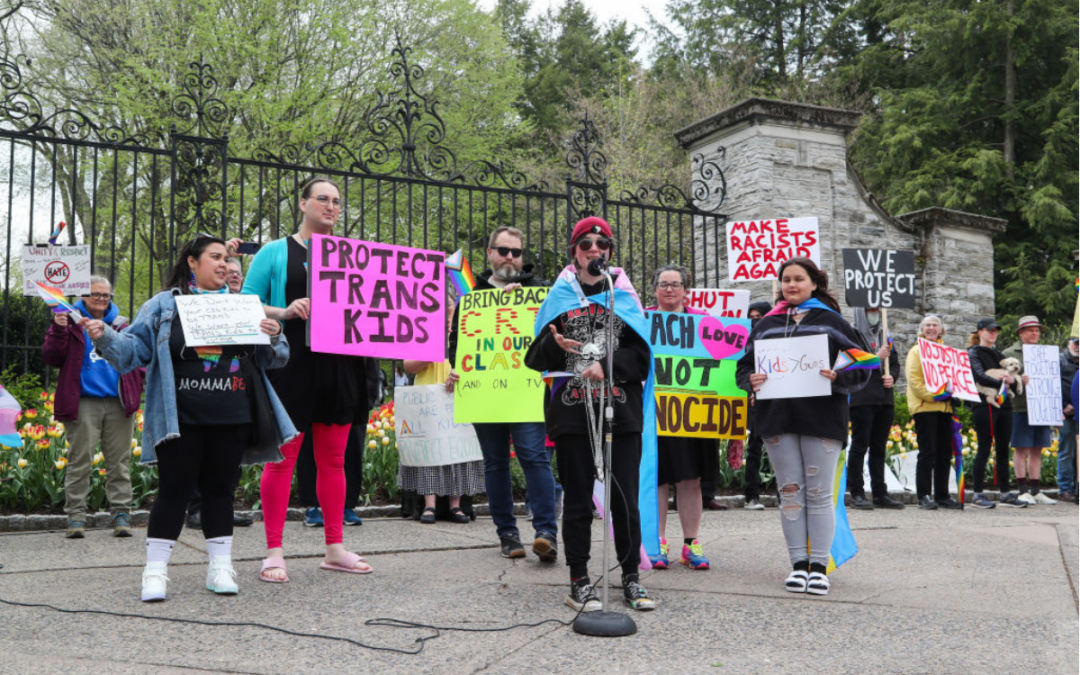
School districts working with anti-LGBTQ groups can cost your kids’ schools millions
Parents across South Central Pennsylvania are worried about the potential financial impacts working with anti-LGBTQ groups may have on their school...

VIDEO: Trump distances himself from his anti-abortion views
Donald Trump appeared on WGAL on Tuesday and continued to distance himself from his anti-abortion views claiming that reproductive rights are now a...

VIDEO: Community pushback gets school board to rescind decision on denying gay actor’s visit
Cumberland Valley School Board offered a public apology and voted to reinstate Maulik Pancholy as a guest speaker a week after the board voted to...

VIDEO: Project 2025 brings nuclear armageddon back into vogue
Project 2025 is a titanic document, with plans ranging from cutting half of all government employees to targeting reproductive rights on a scale...