Pennsylvania is hoping to secure its own slice of a $50 billion rural health fund in the face of federal Medicaid cuts, with a focus on bolstering a beleaguered workforce and expanding health access for more than two million people.
The Rural Health Transformation Fund was a last-minute addition to President Donald Trump’s summer budget bill that imposed Medicaid work requirements and cut upwards of $51 billion in funding to the commonwealth over the next decade. That new fund is worth roughly 37% of the estimated lost Medicaid funding in rural areas.
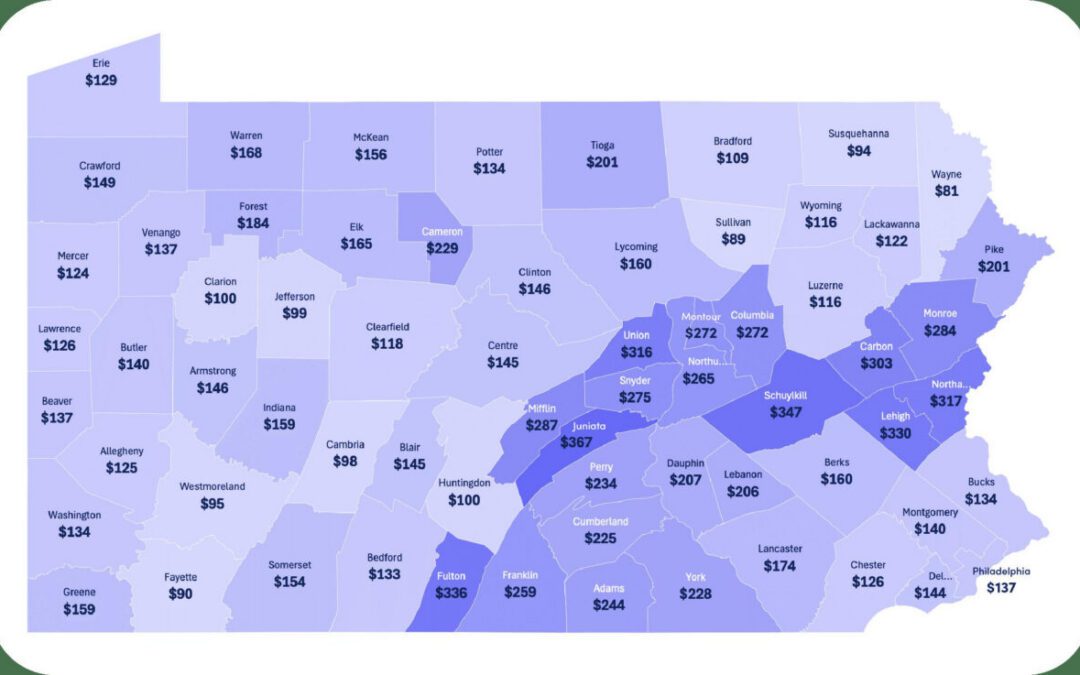
“Pennsylvania is home to the third-largest rural population in the country, and our rural communities face unique challenges when it comes to public health and access to health care. A strong, accessible, affordable health care system is the foundation of any healthy community, and health care is essential to the economic growth, population revitalization, and stabilization of our rural communities,” said Val Arkoosh, the state’s secretary of the Department of Human Services, in a release.
The 67-page application — released Thursday, which was also National Rural Health Day — requests up to $200 million in annual funding over the next five years, totaling $1 billion. Its six focuses include: technology and infrastructure, workforce, maternal health services, behavioral health services, aging and access, and emergency medical services and transportation.
The U.S. Department of Human Services is expected to award funding by the end of the year.
Key objective targets are:
- Access to care: More than 85% of Pennsylvanians can get a routine primary care appointment within four weeks and urgent care appointments within one week.
- Digital connectivity and telehealth: More than 85% of rural hospitals and clinics will have broadband and telehealth functionality. More than 50% of rural hospitals and clinics connected via Fast Healthcare Interoperability Resources.
- Workforce adequacy: Reduce rural hospital vacancy rates by 10% for key direct care roles. Add three new rural training programs.
- System sustainability: More than 60% of systems partnered with rural Community Health Centers for specialty care.
- Health outcomes: Reduce the number of pregnant women living in rural areas with inadequate prenatal care by 20%.
“The state did sort of have their hands tied on the different areas that they could apply for because of the way that (the Centers for Medicare and Medicaid Services) set up that funding,” said Helen Hawkey, the board president of the Pennsylvania Rural Health Association.
She also serves as the director of the Pennsylvania Coalition for Oral Health and added that she would have liked to see more funding for dental access. But the overall investment in workforce development — a need across health care sectors — will attempt to fill in gaps across the spectrum alongside a separate state Rural Health Plan.
“You have to have providers to have access. You cannot access health care if you have no one to provide it,” said Hawkey. “The incentives that are included in the plan — like scholarships, stipends, housing — all of those things are going to be really, really important to try to increase providers in rural areas.”
Shoring up workforce, technology improvements
Though nearly 20% of the state’s population is rural, only 10% of the state’s physicians and hospital beds are in rural counties.
Dentists number even fewer, with just 6% of the state’s practitioners in rural areas.
Additionally, one-third of the state’s rural hospitals are at-risk of closing, according to The Hospital and Healthsystem Association of Pennsylvania. HAP told the Capital-Star in a statement that the anticipated funds wouldn’t be sufficient to make up for lost Medicaid funding.
“Fewer than half of the commonwealth’s rural hospitals are operating with margins necessary for long-term stability because they have been chronically underfunded for the care they provide. Medicaid is among the largest payors for many rural hospitals, yet, in Pennsylvania, reimburses only 71 cents per dollar spent providing care,” said Nicole Stallings, the organization’s president and CEO.
“This is already unsustainable but upcoming federal cuts will reduce reimbursement even more — to 64 (cents) per dollar — resulting in a nearly $1 billion direct payment cut to Pennsylvania’s rural hospitals over the next decade on top of a sharp rise in uncompensated care due to coverage losses.”
The state hopes to use the federal dollars to bolster the workforce of rural hospitals and update technology, both aspects praised by HAP and included in the organization’s September recommendations.
The scholarships, rotations and residencies for future health care practitioners come with a five-year service commitment, prioritizing students from rural backgrounds
The state requested $239.2 million in workforce investments.
The application also pitches telehealth and virtual provider visits as ways to relieve burnout and increase access to specialists, with new technology assistance managed by a central hub. It specifically named artificial intelligence as an opportunity.
Examples include conversational AI, digital check-in tools and chronic disease prevention or management services. The Guthrie Clinic’s Pulse Center in Pennsylvania is highlighted for its use of AI in centralized digital monitoring and improved care coordination, which “ease staff workload and achieve reductions in nurse turnover and hospital costs.”
Even as practitioners report fewer hours devoted to paperwork because of AI, state lawmakers have recently sought to control the growth of AI in health care settings, citing transparency concerns.
A focus on maternal and elder health
Mothers and mothers-to-be have inadequate prenatal care in rural areas, and nearly one-third of rural women live more than 30 minutes away from the closest labor and delivery unit. Three rural hospitals in the state closed their labor and delivery units last year, exacerbating the problem.
The state proposes regional rural Maternal Health Hubs, places where pregnant Pennsylvanians can get comprehensive, coordinated care. The hubs will also facilitate — through face-to-face contact or telehealth — mental, oral and behavioral health care alongside substance use disorder services.
“The hub model is invaluable in rural areas, where patients often face long travel distances, workforce shortages and fragmented care systems,” read the application. “The hub will augment the capacity of existing providers by centralizing key activities and expanding services where gaps exist.”
Investments from the federal government could additionally fund: an app for new moms that connects them to local providers, telehealth and community resources; remote psychiatric and substance use consultations; and remote patient monitoring for high-risk pregnancies or postpartum complications.
For these services, the state is requesting $187.4 million.
Expanding paramedicine services, where specially trained paramedics check on newly discharged patients, could improve recovery times for seniors and reduce readmissions. The providers can assess homes for fall risks — one of the leading causes of hospitalizations for older Americans — and assist with chronic disease management or wellness checks.
Additional dollars could be used to improve nursing home quality and staffing, which fell following the COVID-19 pandemic. In total, the state seeks $77.6 million for aging-related services.
And while the public can expect annual state reports, staff at the University of Pittsburgh Medicaid Research Center will also provide independent evaluations, including “secret shopper” surveys to measure the impacts of rural health investments on appointment availability and wait times.