Inside the hot zone medical staff monitor and treat sick patients infected with the Covid-19 virus at the UMASS Memorial DCU Center Field Hospital in Worcester, Massachusetts on January 13, 2021. - The field hospital currently has fifty non critical patients infected with the Covid-19 virus. The center was set up to relieve hospitals during the surge and allow for non critical patents to free up beds at the main hospital locations. Patients come from around the state to stay at the field hospital. (Photo by JOSEPH PREZIOSO/AFP via Getty Images)
Nearly 4,200 people died from COVID-19 on Tuesday, as a massive spike in infections continues to fill hospitals in the country.
The United States set a grim record on Tuesday as the country recorded the most COVID-19 deaths in a single day since the start of the pandemic.
By Tuesday evening, 4,197 deaths were reported, according to data collected by Johns Hopkins University. The number is expected to grow as overnight data is officially reported. The number of deaths across the country has gone above 4,000 only one other time, on Jan. 7 when the US broke its previous record, with 4,194 deaths.
The United States is continuing to experience a massive spike in new infections. Over the past week, there have been an average of 248,650 new COVID-19 infections each day.
The ongoing spike in COVID-19 deaths and infections coincides with concerns about the slow vaccination rollout. Earlier this week the Trump administration announced that it would release all available doses of coronavirus vaccines, instead of maintaining half of the supply to guarantee everyone who got a first shot will also get a second shot.
The influx of available vaccines comes with orders for states to vaccinate everyone over the age of 65 and adults with underlying medical conditions that place them at a higher risk of dying from the virus. Government officials also said that if states do not use their allocations quickly, they will be given fewer doses in the future. However, it is unclear whether that strategy will be used by the Biden Administration when he takes office on Jan. 20.
In the meantime, hospitals across the country are fighting the rising tide of patients who need medical help. Data from the New York Times shows that about one-fifth of hospitals with intensive care units in the United States are reporting occupancy levels of 95% or more.
Although doctors and medical personnel have improved outcomes for patients with COVID-19, overwhelmed hospitals make treatment more difficult. According to a study from MedRxiv, when intensive care units are full patients have a 92% increased risk of death from the virus. The study has yet to be peer-reviewed.
In short, this could mean that when hospitals are stretched thin, severely ill patients are more likely to succumb to the virus.
Hospitals at capacity are also dangerous for other serious, yet treatable health problems. People who need treatment for injuries, heart attacks, or strokes, for example, are less likely to get the time and treatment that they need because medical personnel are so busy.
“When the hospital fills up, everything gets disrupted and a kind of ‘soft rationing’ kicks in,” Lakshman Swamy, who serves with the Cambridge Health Alliance, told Vox. “The ICU has to raise the bar on how sick you need to be to get into the ICU. If you add stretched out staff … you end up basically providing slower, less ideal care to everyone, including the sickest patients.”

For Rep. Susan Wild, supporting PA families includes reproductive rights and much more
Rep. Susan Wild wants to be very clear with Pennsylvanians: Donald Trump is committed to taking away women’s reproductive freedom, but he is not...
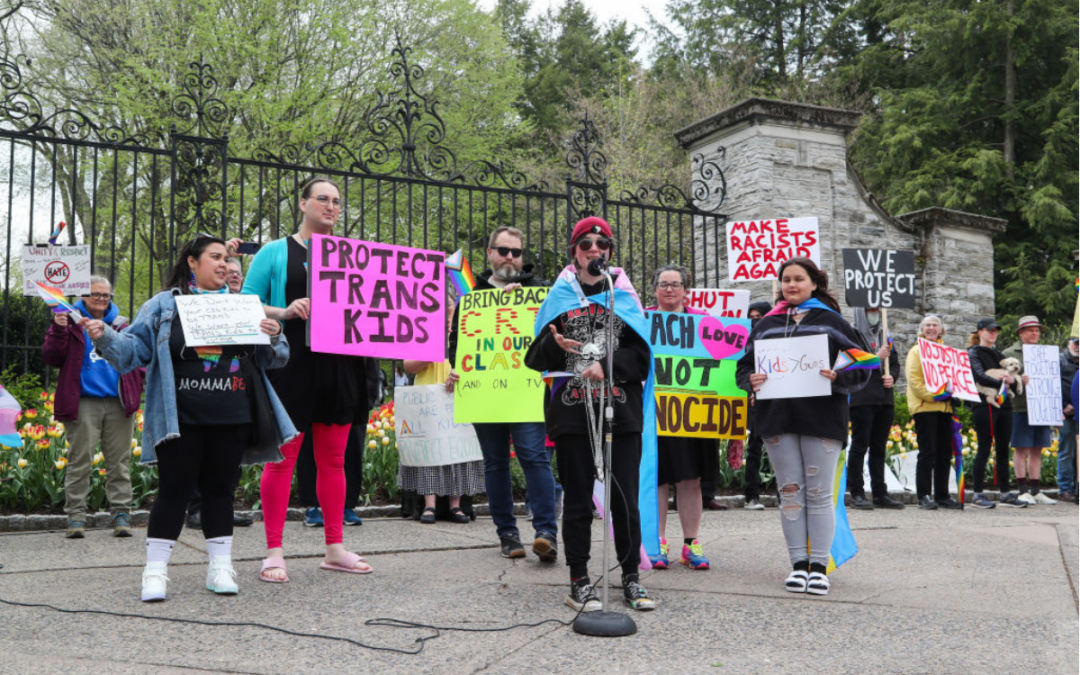
School districts working with anti-LGBTQ groups can cost your kids’ schools millions
Parents across South Central Pennsylvania are worried about the potential financial impacts working with anti-LGBTQ groups may have on their school...

VIDEO: Trump distances himself from his anti-abortion views
Donald Trump appeared on WGAL on Tuesday and continued to distance himself from his anti-abortion views claiming that reproductive rights are now a...

VIDEO: Community pushback gets school board to rescind decision on denying gay actor’s visit
Cumberland Valley School Board offered a public apology and voted to reinstate Maulik Pancholy as a guest speaker a week after the board voted to...

VIDEO: Project 2025 brings nuclear armageddon back into vogue
Project 2025 is a titanic document, with plans ranging from cutting half of all government employees to targeting reproductive rights on a scale...