Issues already prevalent in rural Pennsylvania have helped to spread the virus and increase mortality rates.
The rural way of life is allowing the novel coronavirus to spread faster and kill more people in rural communities than in urban communities, health experts say.
Rural areas are isolated, with not much movement in and out of communities. So, during the first wave of the pandemic in the spring/summer months, it seemed these populations were almost immune, as the number of cases and mortality rates remained low, said Lisa Davis, director of the Pennsylvania Office of Rural Health.
“Rural residents started to feel a sense of safety,” said Dr. Rutul Dalal, Medical Director of Infectious Diseases at UPMC in the Susquehanna Region. “They started to let their guard down, thinking it wasn’t going to reach their community. They also probably got tired of social distancing and wearing masks, since they viewed the virus as an urban problem.”
Dr. Casey Pinto, assistant professor of public health sciences at Penn State University’s College of Medicine, grew up in rural Pennsylvania and agreed with Dalal’s assessment. Pinto said the mentality among rural residents tends to be “if I didn’t see it or it hasn’t directly affected me, it’s not a problem.”
So rural Pennsylvanians continued living the way they always do, and didn’t wear masks while outside among people, Davis said.
What normally is the “neighborly” thing to do, helping others out when they are sick by taking them food or dropping by to check on them, is the exact opposite of what should be done during a pandemic, Pinto said. But that’s what folks in rural Pennsylvania do.
And people in rural areas tend to be older, have lower incomes, and have less access to healthcare facilities.
All of these factors have combined to make the coronavirus a problem in rural communities in this second wave of the virus.
Of the more than 500,000 confirmed coronavirus cases in the state since March, 32% were recorded in rural counties.
Rural counties make up just 26% of Pennsylvania’s population.
Since Oct. 1, rural coronavirus deaths account for 57% of those reported statewide.
Rural Pennsylvanians Are Older
Rural Pennsylvanians tend to be older than people in other parts of the state.
In 2018, 19% of the rural population was age 65 and older—slightly higher than the state’s average of 17.4%. The risk for severe illness with COVID-19 increases with age, putting older adults at the highest risk.
Chronic health conditions, such as heart disease, obesity, and diabetes are already prevalent in rural populations, Dalal said, and put individuals at a higher risk of severe illness from the novel coronavirus. Severe illness means a person with COVID-19 might need to be hospitalized, put in intensive care, put on a ventilator to help them breathe, or they might even die.
Rural Pennsylvanians Have Less Income
Davis said the lower socioeconomic status of rural residents—lower median household income, higher rate of uninsured—also plays an important role in their health.
Rural counties had a median household income of $52,160 in 2018, far below the statewide average of $60,891, according to the Department of Health. Urban counties averaged $65,214.
Lack of health insurance is a major barrier to accessing care and is linked to worse health outcomes and higher costs of care. Overall, in 2018, more than 7% of Pennsylvania’s rural population under the age of 65 was uninsured, with most counties in the 7% to 9% range, and Mifflin County having 9.2%. The statewide average was 6.5%.
Rural Pennsylvanians Have Less Access to Healthcare
Pinto said rural residents are also less likely to seek medical care. And when they finally do go, they might have to travel farther for care and the facilities might not have the proper equipment for the illness.
Access to quality healthcare services is important for promoting and maintaining health, and preventing and managing diseases.
But there aren’t many incentives for medical professionals and facilities in rural areas, so there are often shortages, Dalal said.
In 2017, there was one primary care physician for every 1,387 residents of rural counties, while there was one primary care physician for every 775 residents of urban counties, according to The Center for Rural Pennsylvania.
Pennsylvania is home to a total of 154 acute care hospitals. Of those, 66 (43%) are located in rural counties while 88 (57%) are in urban areas.
Seven rural counties don’t have hospitals—Cameron, Forest, Juniata, Perry, Pike, Snyder, and Sullivan.
Rural hospitals face significant financial challenges and operational limitations. These facilities depend on revenue from outpatient services and elective surgeries, Davis said, which have been cancelled or postponed as COVID-19 cases surge.
Reimbursements provided by the CARES Act have dried up. Facilities are operating on tight, shoestring budgets, Davis said.
Staff are stretched thin. When a worker is exposed to or has contracted the virus, they must quarantine. With no backup available, this has a ripple effect throughout the hospital and many suffer, Davis said.
“The healthcare system in general is at its capacity,” Davis said. “Healthcare providers are exhausted. How much longer can we keep going?”
Effects from the pandemic are going to harm every facility in the long run, Pinto said, but rural facilities will bear the brunt.
“Doctors that may have been treating patients for decades could retire or move away because they are burned out from the pandemic,” Pinto said. “Rural patients, who already don’t access enough preventative care, will lose their primary care physician. Losing one provider in an urban setting is not as big of a problem as in a rural area.”
Support Our Cause
Thank you for taking the time to read our work. Before you go, we hope you'll consider supporting our values-driven journalism, which has always strived to make clear what's really at stake for Pennsylvanians and our future.
Since day one, our goal here at The Keystone has always been to empower people across the commonwealth with fact-based news and information. We believe that when people are armed with knowledge about what's happening in their local, state, and federal governments—including who is working on their behalf and who is actively trying to block efforts aimed at improving the daily lives of Pennsylvania families—they will be inspired to become civically engaged.


For Rep. Susan Wild, supporting PA families includes reproductive rights and much more
Rep. Susan Wild wants to be very clear with Pennsylvanians: Donald Trump is committed to taking away women’s reproductive freedom, but he is not...
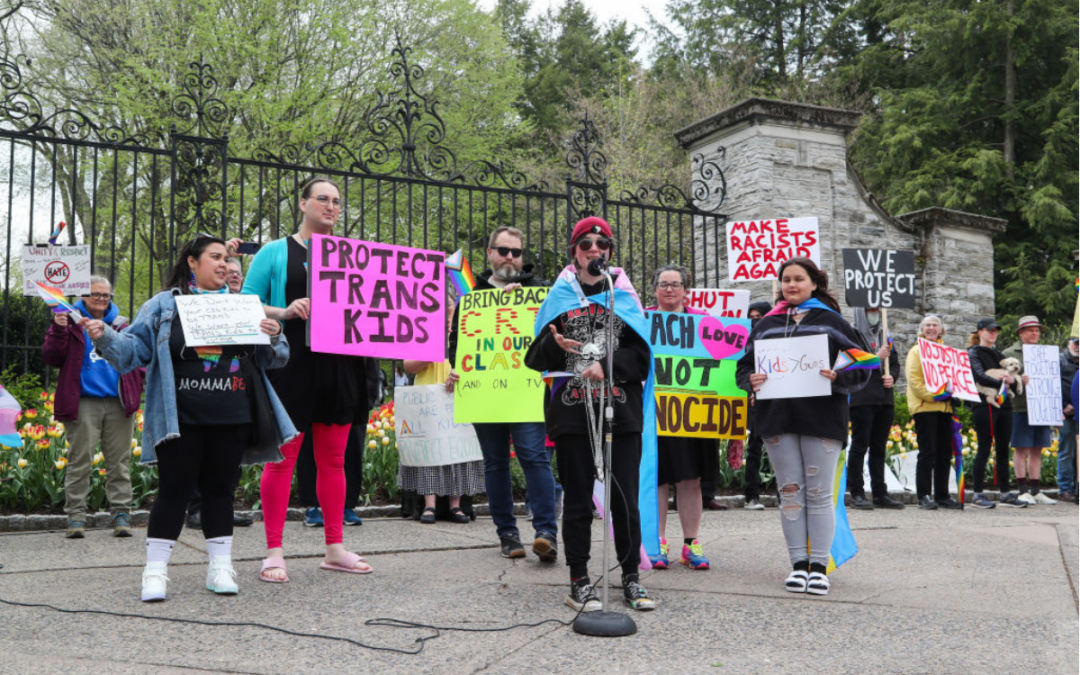
School districts working with anti-LGBTQ groups can cost your kids’ schools millions
Parents across South Central Pennsylvania are worried about the potential financial impacts working with anti-LGBTQ groups may have on their school...

VIDEO: Trump distances himself from his anti-abortion views
Donald Trump appeared on WGAL on Tuesday and continued to distance himself from his anti-abortion views claiming that reproductive rights are now a...

VIDEO: Community pushback gets school board to rescind decision on denying gay actor’s visit
Cumberland Valley School Board offered a public apology and voted to reinstate Maulik Pancholy as a guest speaker a week after the board voted to...

VIDEO: Project 2025 brings nuclear armageddon back into vogue
Project 2025 is a titanic document, with plans ranging from cutting half of all government employees to targeting reproductive rights on a scale...